National Cancer Centre Singapore will NEVER ask you to transfer money over a call. If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Neurofibromatosis type 1
What is Neurofibromatosis type 1?
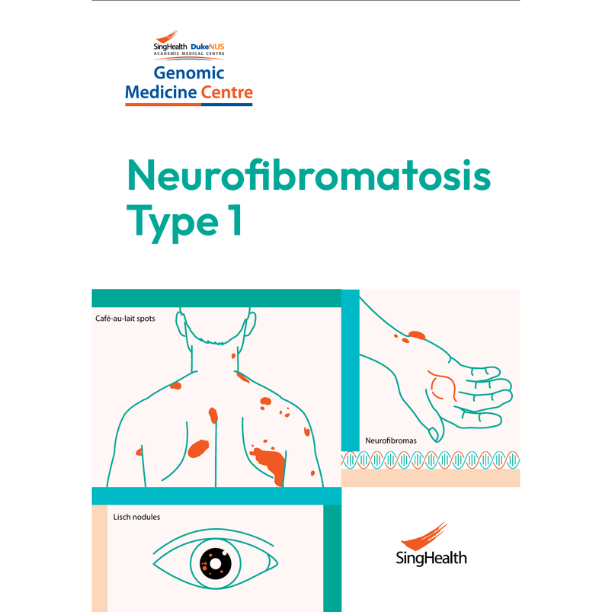
Neurofibromatosis type 1 (NF1) is a hereditary condition commonly associated with multiple Café-au-lait (light brown) spots on the skin and tendency to grow neurofibromas (benign tumours). Neurofibromas are often seen as raised bumps on the skin and can occur anywhere on the body. While these skin changes do not have serious medical consequences, they can affect a person's appearance. Individuals with NF1 may be at increased risk of other conditions like high blood pressure or cancer and would benefit from early screening and intervention.
How common is NF1?
NF1 is among the most common genetic conditions. It is estimated that as many as 1 in 3,000 people have NF1. This condition has been observed in all racial groups and affects both genders.
What are the features of NF1?
Individuals with NF1 may have different features, and no one person will have the symptoms of NF1. The severity of symptoms can range from extremely mild to severe, and can vary within individuals of the same family as well. There is no way to predict who will have a mild case or who will develop more serious symptoms, but majority of individuals (60%) usually experience minor symptoms.
- Café-au-lait spots
These are flat, light brown, coffee-coloured patches on the skin that are not harmful.
Individuals with NF1 usually have six or more of these spots on their body. - Neurofibromas
- Neurofibromas are pea-sized bumps that can grow on the skin surface or under the skin and very commonly seen in people with NF1.
- The number of neurofibromas in individuals with NF1 can vary greatly, from just a few to hundreds.
- Most are not medically concerning, but can cause pain and itching.
- Plexiform neurofibromas are larger and deeper tumours around the nerves.
- These are also benign tumours that can grow quite large and can cause medical problems, affecting structure of the nearby bone, skin and muscle.
- These types of neurofibromas can become cancerous in 10% of cases.
- Optic glioma
- A tumour along the optic nerve in the brain
- 15% of children with NF1 may develop an optic glioma, usually before the age of 6.
- Most do not cause any symptoms, but some can affect vision and may require treatment.
- Lisch nodules
- The appearance of tiny tan clumps of pigment within the iris of the eyes, that does not affect vision and does not require treatment.
- Scoliosis
- This is known as the curving of the spine, which is common in people with NF1.
- In most cases, it is mild and appears during the teenage growth spurt.
- Bone issues
- Some people with NF1 have bone defects from birth
- These defects can occur in almost any bone, most commonly seen in the skull and limbs like
- Bowing of the leg bones below the knee occurs in about 5% of people with NF1
- Cognitive differences
- Intelligence in NF1 is usually in the normal range, but children may need extra support in school.
- Learning challenges occur in about 50% of children with NF1.
- Delayed or early puberty
- Most will start puberty during the expected age range, but some may experience early or delayed puberty.
- High blood pressure (hypertension)
- For a minority of people with NF1, hypertension is one of the serious complications of NF1.
- People with NF1 should have their blood pressure checked annually.
How is NF1 diagnosed?
Only a physician can make a formal diagnosis of NF1. The diagnostic criteria for NF1 were updated in 2021, and the updated criteria are listed below. In order to make a diagnosis of NF1, an individual must have two or more of the following:
- Six or more café-au-lait macules
- Freckling in the axilla (armpit) or groin
- Two or more neurofibroma tumours of any type or one plexiform neurofibroma
- Two or more Lisch nodules or two or more abnormalities in the choroid (vascular layer of the eye)
- Optic pathway glioma
- Osseous lesion (bony lesion), such as sphenoid dysplasia (abnormal growth) of the bone behind the eye, or dysplasia or pseudarthrosis of the tibia (long bone in the leg) or other long bones
- A faulty NF1 gene found by genetic testing
- A family member with NF1
What causes NF1?
NF1 is a genetic condition, which means this condition can be passed from generation to generation in a family. It is caused by a fault (i.e. mutation) in the NF1 gene. Genes are instructions for cells to make proteins in the body. The NF1 gene is a tumour suppressor gene which normally produces protein to block the development of tumours and cancer. When faulty, it leads to a diagnosis of NF1 and an increased risk of cancer/tumours.
You can undergo genetic testing to understand if you have a faulty NF1 gene, but it is a personal choice. Genetic testing can be informative for other family members or to guide reproductive options. It can also help to further confirm a genetic diagnosis, or help to diagnose a young child who has not yet developed enough signs to make a clinical diagnosis of NF1. Genetic testing cannot predict the severity or specific complications in any individual case of NF1. A genetics healthcare provider or genetic counsellor can help you make a decision on whether to have testing.
If your personal or family medical history is suggestive of NF1 that has yet to be diagnosed, please talk to your doctor. A referral to a genetics clinic can help you find out more.
What can be done to manage NF1?
Because NF1 can affect different parts of the body, and symptoms can vary from person to person, doctors and healthcare professionals from different specialities may be involved in the care of NF1 patients. This may include dermatologists, neurologists, ophthalmologists, orthopaedists, oncologists, cardiologists and genetic counsellors. These doctors will help manage risk and symptoms that come with NF1.
Additionally, ongoing research is focused on ways to identify drugs and therapies for people with NF1. These treatments include the shrinking or halting of the growth of neurofibromas associated with NF1. Furthermore, NF1 individuals with cancer can also consider targeted therapies for treatment.
Neurofibromatosis Type 1
Keep Healthy With
© 2026 National Cancer Centre of Singapore Pte Ltd. All Rights Reserved.
















