National Cancer Centre Singapore will NEVER ask you to transfer money over a call. If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Pain
- Allergies
- Appetite Loss
- Bone Problems
- Breathing Problems
- Constipation
- Diarrhoea
- Difficulty Swallowing (Dysphagia)
- Dry Mouth (Xerostomia)
- Difficulty Sleeping (Insomnia)
- Feeling Tired (Fatigue)
- Fevers and Infections
- Hair Loss
- Heart Problems
- Menopausal Symptoms
- Indigestion
- Joint Pains
- Limb Swelling (Lymphedema)
- Muscle Aches
- Nail Changes
- Nausea and Vomiting
- Pain
- Tingling or Numbness in Hands or Feet (Peripheral Neuropathy)
- Skin Changes
- Sore Mouth (Oral Mucositis)
- Taste Changes

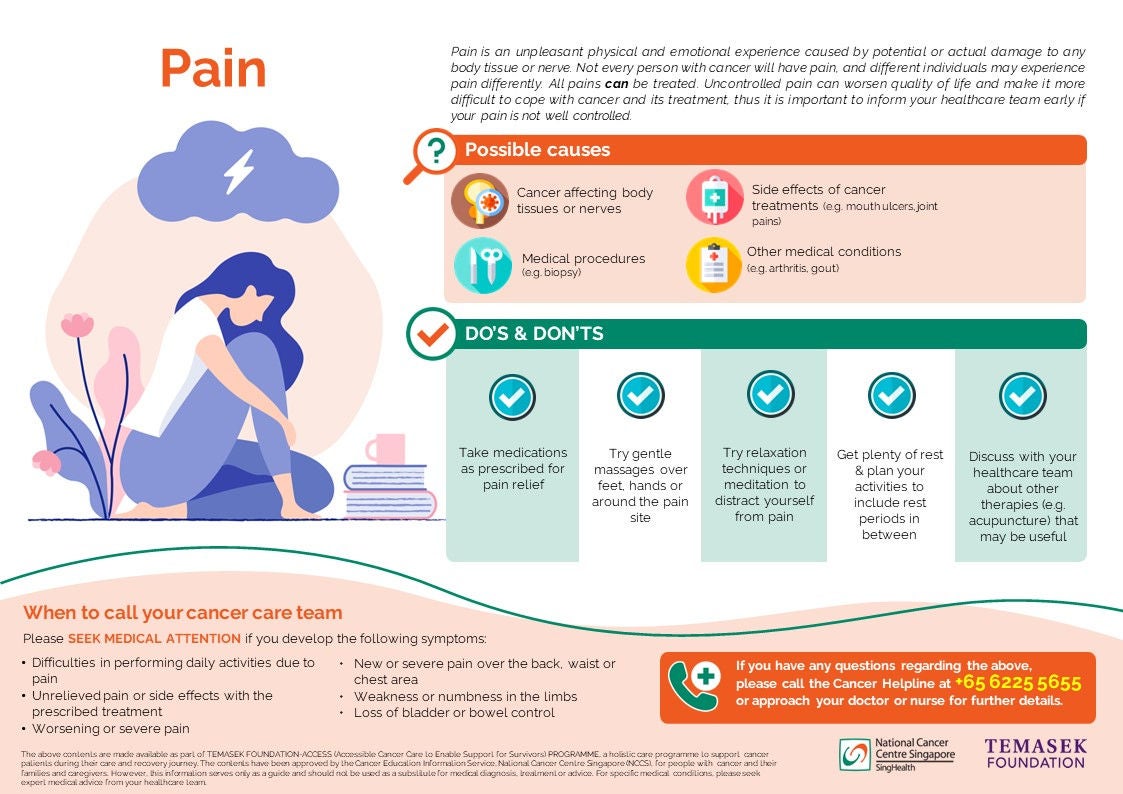
Pain is an unpleasant sensation and experience caused by damage to any body tissue or nerve. Although it may seem common, not every person with cancer will experience pain. Even if you do, it may help to know that all pains can be treated, and most pains can be controlled. If left untreated, pain can lead to other distressing problems such as insomnia, depression, fatigue and difficulties in carrying out your daily activities normally. As uncontrolled pain can make it more difficult to cope with cancer and its treatment, you are advised to report any pain to your doctor or nurse early.
Causes of Cancer Pain
- Direct effect of cancer damaging or affecting body tissues or nerves
- Medical investigations used to diagnose cancer and determine the effects of cancer treatment (e.g. bone marrow test, biopsy) can cause some discomfort at the site where the test is done.
- Cancer treatment
- Surgery. It is normal to have pain over the surgery site. This type of pain usually subsides after the wound heals. Some people however can experience pain even after the wound heals, due to scarring at the operation site.
- Chemotherapy, hormonal therapy. Certain types of chemotherapy (e.g. oxaliplatin, paclitaxel) can cause pain and numbness in the fingers or toes (see peripheral neuropathy), which often goes away after treatment finishes. In some cases however, this side effect may need long term management. Hormonal therapy may sometimes cause joint pains and muscle aches.
- Radiation therapy. Depending on the radiation dose and area, pain can be one of the side effects. For instance, radiation to the head and neck causes mouth ulcers which can be painful. This, again, will improve upon completion of the treatment.
People with cancer can also experience pain that is not directly linked to the cancer or its treatment (e.g. pain from arthritis or migraines). At times, non-physical stresses such as anxiety or other emotional stresses, or even social or work problems can make your pain feel worse. This means that it is just as important to manage these other stresses together with treatment for the physical causes of pain, so that you will be able to cope better with the pain.
What you need to look out for
The cause and experience of pain differs from person to person. Some symptoms that may occur include:
- Pain in any area of the body
- Inability to carry out normal activities due to pain
- Fatigue and/or low mood due to pain
How it can be treated
As treatment of pain depends on its cause, your doctor will ask you more questions regarding your pain (e.g. when it first started, how it feels like) and perform a physical examination to find out what is causing the pain. Your doctor may also advise for further investigations (e.g. x-rays) if needed. Based on your condition and cause of pain, your doctor will:
- Treat the underlying cause wherever possible. If the tumour is causing pain directly, using anticancer treatments like chemotherapy or radiotherapy can shrink the tumour and help reduce pain.
- Prescribe medications for pain relief. These may include painkillers (e.g. paracetamol, opioids like tramadol, morphine, etc.), or other medications (e.g. corticosteroids to help reduce inflammation, muscle relaxants for muscle pains, nerve stabilizing medications for painful peripheral neuropathy etc.).
- Use other methods for pain relief. In some instances, injecting substances into painful nerves (nerve block) or procedures to strengthen painful bones (vertebroplasty, kyphoplasty) can also be helpful.
- Refer to other healthcare professionals to help treat pain or its complications. These may include a pain or palliative care specialist to further manage your pain, or other healthcare professionals (e.g. social workers, psychologists, physical therapists) to help you cope better with your pain in your daily life.
What you can do
The first step to successful pain management is to inform your doctor or nurse as soon as you experience it. Here are some further steps you can take, as you work with your healthcare team to prevent or treat your pain:
Keep track of your pain
|
|
Follow your treatment regimen
|
|
Try non-drug therapies for pain relief
|
|
When to call your cancer care team
Please inform your doctor or nurse as soon as you develop the following symptoms that may indicate worsening or complications of the condition.
- Your pain is not relieved with the prescribed treatment
- Your pain makes it difficult for you to eat, sleep or perform your normal daily activities
- You have side effects from the medications prescribed for your pain
- You develop severe pain
- You develop new or severe back pain with the following symptoms:
- Weakness/ numbness in the lower body
- Pain around waist or chest
- Loss of bladder/ bowel control
- The above indicates possible spinal cord compression, a MEDICAL EMERGENCY which requires IMMEDIATE MEDICAL ATTENTION: please go to your nearest hospital as soon as possible. Delayed treatment may result in long term disability.
For more information on cancer pain, medications used for pain and myths about morphine, you may refer to the booklet on “NCCS Cancer Pain and its management: A guide for patients, families and caregivers” . If you have any questions regarding the above, please call the Cancer Helpline at +65 6225 5655 or approach your doctor or nurse for further details.
Click here to download the PDF version of this article.
如果您要下载本文的中文版本,请点击此处。
Klik di sini untuk memuat turun versi PDF artikel ini.
The above contents are made available as part of TEMASEK FOUNDATION-ACCESS (Accessible Cancer Care to Enable Support for Survivors) PROGRAMME, a holistic care programme to support cancer patients during their care and recovery journey.
The contents have been approved by the Cancer Education Information Service, National Cancer Centre Singapore (NCCS), for people with cancer and their families and caregivers. However, this information serves only as a guide and should not be used as a substitute for medical diagnosis, treatment or advice. For specific medical conditions, please seek expert medical advice from your healthcare team.
Brought to you by:
Keep Healthy With
© 2025 SingHealth Group. All Rights Reserved.