Children with congenital heart conditions are often exempted from physical activity, resulting in a relatively sedentary lifestyle which poses various health risks. However, research has discovered that with the right approach, these children can benefit from physical activity as part of an individualised, safe and appropriate plan.
INTRODUCTION
Congenital heart disease (CHD) is a common birth defect with a prevalence of nine in 1,000 live births in Singapore.1 A significant portion of these patients requires regular clinical follow-ups and surgical interventions in early childhood.
As survival rates improve with surgical advances in congenital heart surgery and medical technologies, research into physical activity for patients with congenital heart defects has shown benefits of appropriate moderate physical activity, over the risks of a sedentary lifestyle including obesity, exercise intolerance, acquired cardiovascular diseases and
psychosocial morbidities.2
In Singapore, children with CHD are often exempted from various forms of physical activity from early childhood and throughout their schooling years, leading to a relatively sedentary lifestyle. These restrictions may be secondary to actual clinical concerns such as outflow tract obstructions, pulmonary vascular diseases or arrhythmias.
However, in many cases, limitations are imposed due to parental and educational institutional concerns, or a lack of clinical understanding of the actual physical and exercise recommendations for the underlying condition.
Medical practitioners play an important role in educating and counselling for appropriate active participation in physical activity during consultation for children with CHD. Recent consensus guidelines have recommended that children with CHD “comply with public health recommendations of daily participation in 60 minutes or more of moderate-to-vigorous physical activity (MVPA) that is developmentally appropriate and enjoyable and involves a variety of activities.” 3 |
It is important to recognise that these guidelines distinguish physical activity from exercise.
Physical activity is a broader concept that incorporates “any bodily movement produced by skeletal muscles that results in energy expenditure” and includes activities such as walking and stair climbing.
Whereas, exercise is defined as “planned, repetitive and purposeful physical activity designed to improve one or more components of physical fitness”. This comprises a broad range of activities such as aerobic and resistance exercises, leisure-based activities (e.g., cycling, rollerblading), and recreational to competitive sports participation.2
There are already established guidelines specific to competitive sports participation in children and adolescents with CHD. The scope of this article is to provide practical recommendations to promote appropriate physical activity participation in children with CHD.
APPROACH TO PHYSICAL ACTIVITY PROMOTION IN CHD
Promoting physical activity amongst children with CHD needs to take into consideration the multiple factors that can influence participation. Knowing the child’s unique clinical condition and physical function is vital and should be balanced with identifying and addressing common barriers such as parental/family support, level of motivation, activity interests, time, access to equipment and facilities, etc.Gaining an in-depth understanding of the child will help improve the safety and effectiveness of physical activity participation.
The approach to physical activity promotion in children with CHD should include: clinical assessment, physical activity counselling, individualised physical activity plan and follow-up review.
1. Clinical Assessment
Recommendations of physical activities by medical practitioners require a thorough assessment and understanding of the patient’s underlying cardiac condition, as well as presence of any exertional symptoms such as palpitations, excessive dyspnoea and syncope. In addition to non-invasive assessments such as echocardiography and Holter monitoring, formal exercise testing can also be considered to evaluate for cardiovascular risks, to assess changes in the patient’s physiology during exercise and to establish current level of fitness.
Exercise testing, commonly known as exercise stress testing, involves the use of progressively increased workload to evoke physiological changes during exertion, usually at or near
maximal intensity.
During the test, patients are to exercise until they develop symptoms (e.g., dyspnoea, fatigue) that result in the patient being unable to continue further or at a higher workload. When performed with electrocardiogram (ECG) monitoring, the test is useful for detecting exercise-induced rhythm changes and blood pressure responses.
Cardiopulmonary exercise testing (CPET) is similar to standard exercise stress testing.
During this test, ECG monitoring is supplemented with metabolic gas analysis, and provides an objective assessment on the functional capacity of the heart, lungs and peripheral muscle. The test requires the patient to exercise to volitional exhaustion, and physiological parameters such as heart rate, oxygen uptake, and ventilatory thresholds at both sub-maximal and peak exercise intensity are taken.
These readings provide valuable insight into the child’s aerobic capacity, circulatory function and gas exchange efficiency. Information from CPET provides objective measurements which can help in the tailoring of a more individualised physical activity prescription for the patient, and also aid in reassuring both family and patient on their ability to partake in recreational or even competitive sports.4
2. Physical Activity Counselling
Following the clinical evaluation, medical practitioners are encouraged to provide counselling interventions to understand and address concerns pertaining to exercise participation, set realistic goals and provide a management plan for activity participation.
Counselling practices should be based on knowledge about the child’s current physical activity level, which can be assessed using appropriate assessment tools such as pedometers, accelerometers or heart rate monitors. These devices provide objective assessment of habitual physical activity level, including frequency, patterns and intensity of activity participation. While the use of appropriate objective assessment tools is recommended, validated questionnaires such as the International Physical Activity Questionnaire (IPAQ) or structured screening questions like the Physical Activity Vital Sign (PAVS) (Table 1) can provide a quick assessment of a child’s activity and inactivity status.
The conversation on physical activity should ideally involve both child and family, with an aim to create awareness, educate, assess readiness to change and elicit any concerns and barriers regarding physical activity participation.
Awareness & Education
Medical practitioners should promote physical activity participation based on the general guidelines of 60 minutes of moderate-vigorous physical activity (MVPA) daily.
Activities can range from active transportation and lifestyle or leisure time activities, to healthenhancing activities. Activity time can be built up progressively and accumulated across a day to meet the 60 minutes target.
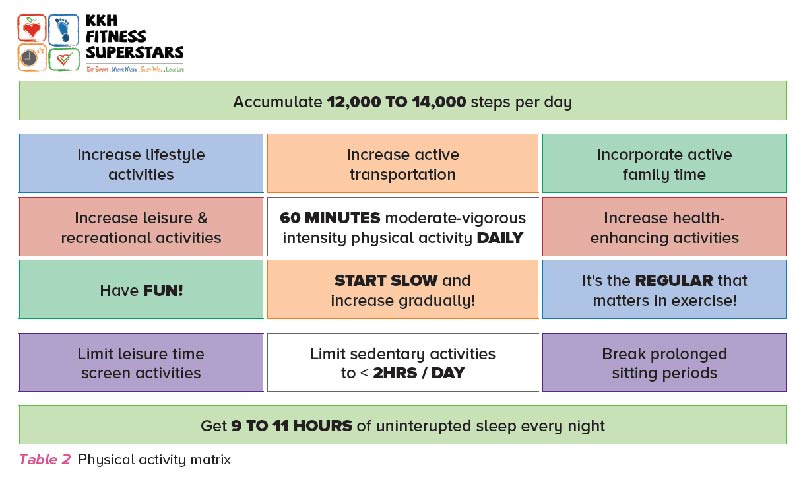
Wearable devices can be used to monitor their daily activity levels. For children, they should aim to accumulate more than 12,000 steps per day. Assure parents of the safety of appropriate physical activity participation for their child, and highlight the health risks associated with prolonged sedentary behaviour.
The physical activity matrix below (Table 2) is a good tool which the child can use to identify areas they can work on to improve their activity levels, evolving the counselling into patient-centred communication. This can be used as an adjunct for addressing physical activity counselling in a busy clinic setting.
Motivation and Barriers
Understanding both the child and parents’ readiness to change is vital in matching activity advice to their motivational level. The next step would be to help them identify perceived barriers which may influence their participation in physical activity.
Common barriers for children with CHD include poor self-efficacy, parental overprotection, social stigma, exclusion by teachers and peers, lack of knowledge and/or access to safe and enjoyable physical activity programmes. Importantly, the counselling practice should aim to help the child address identified barriers and provide realistic solutions to mediate the adoption of, and influence the adherence to, physical activity participation.
Goal Setting
From the in-depth understanding of the child’s motivation and barriers, medical practitioners should work with the child to identify, set and prioritise realistic and measurable physical activity or health goals.
3. Individualised Physical Activity Plan
Information from the clinical assessment and physical activity counselling can be used to provide an individualised physical activity plan. Broadly, the type of physical activities recommended should be developmentally appropriate, and target the key dimensions including fundamental movement skills and exercise improving health-related fitness such as aerobic, resistance and flexibility exercises.
An individualised exercise prescription needs to provide recommendations for appropriate intensity in which physical activity or exercise should be performed. This can be determined objectively from a cardiopulmonary exercise test (CPET) or by calculating relative intensity using age-predicted heart rate formula.
For children with CHD who may have chronotropic incompetence, CPET is recommended, and the target exercise intensity should be based on the workload or heart rate determined at the point of ventilatory threshold identified from the test. Where CPET services are not available, target exercise intensity can be determined using a relative intensity method basing on the agepredicted formula: 207 – 0.7x age.
For most children with CHD, commencement of physical activity at low-to-moderate intensity (50-70%HRmax) is encouraged. Participation in vigorous intensity activities (>70%HRmax) should be introduced gradually and done after a review of their exercise tolerance and fitness. Consideration for higher intensity activities should be based on the underlying physiological function, which can vary with CHD diagnosis and the nature of the exercise or sport.
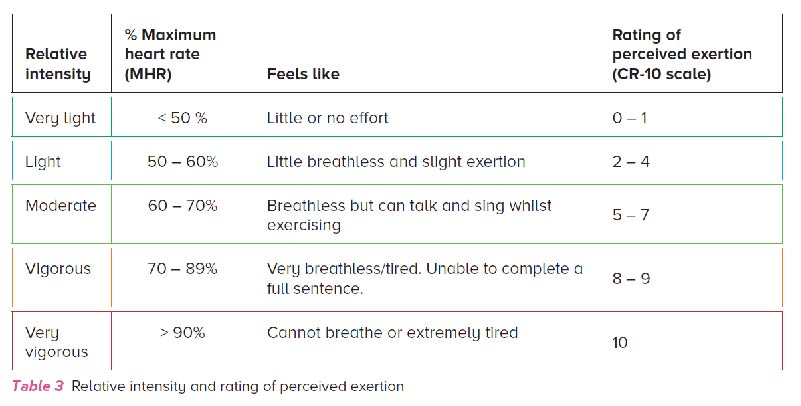
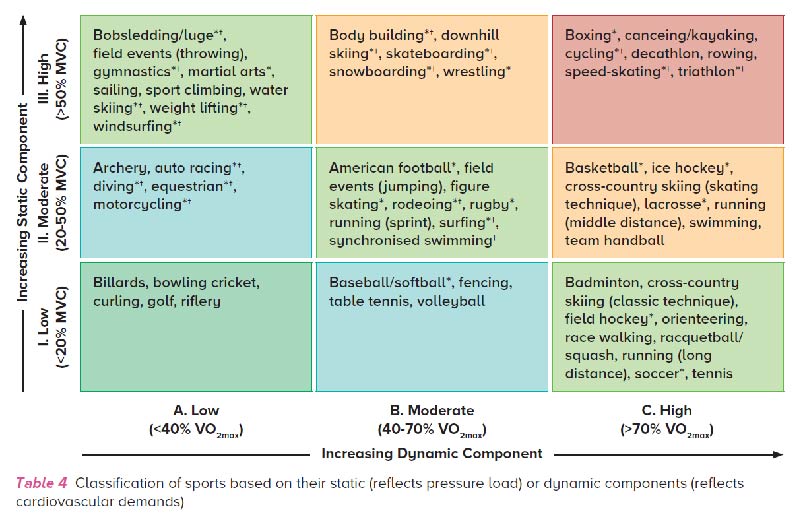
Table 4 shows the classification of sports based on their static (reflects pressure load) or dynamic components (reflects cardiovascular demands). The lowest total cardiovascular demands (cardiac output and blood pressure) are shown in green and the highest in red.3
4. Follow-Up Review
Follow-up review of the child’s physical activity or exercise prescription is important. The child should be asked about their physical activity experience, specifically if there were any issues that may require adjustments or further evaluation before continuing. For children who have undergone cardiopulmonary exercise evaluation, these should be repeated every
two to three years to assess for changes in physiological function before reviewing their activity plan.
CONCLUSIONChildren with CHD can participate in and benefit from physical activity and exercise. Formal exercise testing can help provide an objective assessment of the child’s functional capacity. Child-centred physical activity counselling will be useful for understanding motivation and barriers, and assisting the medical practitioner in formulating a safe and appropriate physical activity plan. |
REFERENCES
- Ngeow A, Tan M, Tan W, et al. PO-0503 Ten Year Study Of Prevalence And Diagnosis Of Congenital Heart Disease (chd) In An Asian Country: Implications On Antenatal Diagnosis And Newborn Screening. Archives of Disease in Childhood 2014;99:A412-A413
- Longmuir PE, Brothers JA, de Ferranti SD, Hayman LL, Van Hare GF, Matherne GP, Davis CK, Joy EA, McCrindle BW; on behalf of the American Heart Association Atherosclerosis, Hypertension and Obesity in Youth Committee of the Council on Cardiovascular Disease in the Young. Promotion of physical activity for children and adults with congenital heart disease: a scientific statement from the American Heart Association. Circulation. 2013;127:2147–2159
- Takken, T. & Giardini, Alessandro & Reybrouck, Tony & Gewillig, Marc & Hovels-Gurich, Hedwig & Longmuir, Pat & McCrindle, B & Paridon, S & Hager, A. (2012). Recommendations for physical activity, recreation sport, and exercise training in paediatric patients with congenital heart disease: a report from the Exercise, Basic & Translational Research Section of the European Association of Cardiovascular Prevention and Rehabilitation, the European Congenital Heart and Lung Exercise Group, and the Association for European Paediatric Cardiology.. European journal of preventive cardiology. 19. 1034-65.
- Budts W, Borjesson M, Chessa M, van Buuren F, Trindade P, Corrado D, et al. Physical activity in adolescents and adults with congenital heart defects: individualized exercise prescription. Eur Heart J. 2013;34(47):3669–74.
Dr Micheal Lim is currently Head & Principal Clinical Exercise Physiologist in Sports Medicine at KK Women’s and Children’s Hospital (KKH). He has been instrumental in the development of clinical exercise physiology services for both paediatrics and adult women in KKH. With over 13 years of clinical experience, he has established various clinical exercise intervention programmes for women and children with weight issues, chronic health conditions and special developmental needs. He is passionate about the field of preventive health, and strongly believes that exercise is an integral pillar of disease prevention and health optimisation.
Dr Dyan Zhang is a Consultant Paediatrician at KK Women's and Children's Hospital subspecialising in Paediatric Cardiology. She is a Clinical Physician Faculty Member of the SingHealth Paediatrics Residency Programme, Clinical Lecturer at National University of Singapore (NUS) Yong Loo Lin School of Medicine, Senior Lecturer at Lee Kong Chian School of Medicine and Adjunct Instructor at Duke-NUS Medical School. Her clinical interests include congenital heart defects, cardiomyopathy and heart failure, cardiac stress testing, and child development in congenital heart diseases.
GPs can call the SingHealth Duke-NUS Sport & Exercise Medicine Centre for appointments at the following hotlines:
Singapore General Hospital: 6326 6060
Changi General Hospital: 6788 3003
Sengkang General Hospital: 6930 6000
